- Information
- AI Chat
Adult Health 1 Quiz 1
Adult Health I (NR-324)
Chamberlain University
Recommended for you
Preview text
Adult Health 1 Quiz 1
Fluid imbalances
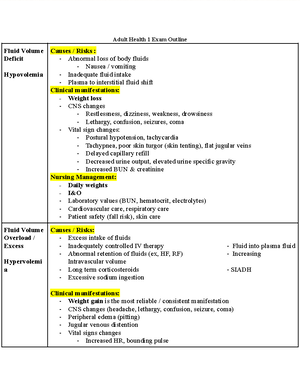
Fluid volume deficit/ Hypovolemia/ Dehydration o Risk factors/Causes Excessive GI loss: vomiting, NG suctioning, diarrhea Excessive skin loss: diaphoresis without water and sodium replacement Excessive renal system losses: polyuria, diuretic therapy, kidney disease, adrenal insufficiency Third spacing: burns Hemorrhage or plasma loss Altered intake: anorexia, nausea, impaired swallowing, confusion, NPO (decreased intake and sodium) o Clinical manifestations Hypotension (orthostatic) HR will be tachycardic and thready Temperature will be decreased Dizziness Syncope Confusion Fatigue Furrow tongue (cracked) Dry mucous membrane Oliguria (less than 30ml/hour) Diminished capillary refill Sunken eyeballs Flattened neck veins Poor skin turgor o Labs Low Hgb ( Normal 12 -16 for women; 13-17 for men ) High SG ( Normal 1 – 1 ) BUN will be higher than 20 ( Normal 10-20 ) Increased Hct ( Normal 36-44% for women; 41-50% for men ) Increased blood osmolarity Specific Gravity o Nursing Interventions Assess for clinical manifestations of FVD Monitor weight and VS, including temperature Assess skin turgor Monitor fluid I&O Monitor lab findings Administer oral and IV fluids as indicated Provide frequent mouth care Implement measures to prevent skin breakdown
Provide for safety (Ex. Provide assistance for a client rising from bed or chair)
Fluid volume overload/ overhydration/ Hypervolemia o Risk Factors/Causes Heart failure (causes dependent edema) Cirrhosis Kidney failure Increased glucocorticosteroids Hypertonic fluids Burns NSAIDs Deficient of ADH (SIADH), Aldosterone, and ANP Excessive sodium intake o Clinical manifestations Tachycardia with a bounding pulse Hypertension Increased central venous pressure Confusion Muscle weakness Altered LOC Paresthesia Visual changes Seizures Increased GI motility Ascites Dyspnea Orthopnea Crackles Pitting edema Distended neck veins Weight gain Skin pallor Dependent pitting edema Pulmonary congestion o Labs Decreased Hct (Normal 32 – 45%) Decreased Na ( Normal 135-145 ) Decreased BUN ( Normal 10-20 ) Low SG ( Normal is 1 – 1) Osmolarity is less than 275 ABG: Respiratory alkalosis Diagnostics (ECG and CXR) Sodium o Nursing Interventions Assess VS, skin turgor, for clinical manifestations of FVO
Caused by deficient metabolic acids, excessive vomiting, hypokalemia,
Guidelines for ABI (these are my notes from patho, shout out to ma girl Makhani!) If the pH is less than 7, it is ALWAYS acidic For both resp acidosis and alkalosis, the pH and PaCO2 are opposite from one another. So, when the pH is high the PaCO2 is low and vice versa. For both metabolic acidosis and alkalosis, the pH and HCO3, follow each other. So when one is low, so is the other.
Forces that move water Osmotic pressure: Inward “pulling force” by plasma proteins from the surrounding tissue into the capillaries
Hydrostatic pressure: Outward “pushing force” pushes fluid out of capillaries to interstitial space
Serum Osmolality 279-
Isotonic: same concentration of blood (275-295): little fluid shift – for acute dehydration & shock [Ex: 0% NS; Lactated Ringers (LR)]
Hypotonic: more dilute then blood (<275); cells swell – for long term dehydration & hypernatremia; Do not use with cerebral edema [Ex: 0% NS; Dextrose 5% water (DSW) (Na free)
Hypertonic: more concentrated than blood (>295); cells shrink – for hyponatremia (& IICP); what is included in assessment? [Ex: D10, D5LR, D5NS, 3% NS, TPN; give D10 when TPN interrupted; colloids: albumin/blood]
Total Parenteral Nutrition (TPN) Nursing Care It is ordered daily and specifically made for each patient. Nothing is added to TPN. It is good for only 24 hours. Refrigerate until half an hour before using Dedicated line (you will need to start a new IV line to administer this) (special filter for TPN & fat solution- change filter & tubing need to be changed daily) It needs to be checked by 2 nurses and be given through IV pump only Site dressing changes – strict aseptic technique Vital signs Q4 hours/ daily weights & laboratory tests/ BG Q4 – 6 hours – sliding scale insulin coverage Monitor for complications: o High risk for infection – bacteriostatic o Hyperglycemia/ Hypoglycemia/ Fluid Volume Overload o Catheter patency/ Catheter - related infection/ Septicemia
Potassium Potassium normal level is 3 – 5 Potassium is cardiac sensitive
Hypokalemia (less than 3)
Risk factors/causes for low potassium
Your body is trying to “DITCH” K+ D rugs (diuretics, corticosteroids) I nadequate intake of K+ T oo much water intake (dilutes the K+) C ushing syndrome – retains Na, excretes K+ (increase in secretion of Aldosterone) H eavy Fluid loss (K+): Vomiting, diarrhea, NG suctioning, ileostomy drainage, polyuria, sweating Glucose in urine pulls K+ into cells – insulin Alkalosis
Expected findings (low and slow) Cardiovascular o Thready, weak, irregular pulse o Weak peripheral pulse o Orthostatic hypotension o Dysrhythmias o ECG changes: ST depression, flat or inverted T wave, prominent U wave (this is abnormal) Respiratory o Shallow, ineffective respirations that result from profound weakness of the skeletal muscles of respiration o Diminished breath sounds Neuromuscular o Anxiety, lethargy, confusion, coma o Skeletal muscle weakness, leg cramps o Loss of tactile discrimination o Paresthesia o Deep tendon hyporeflexia GI o Decreased motility, hypoactive to absent bowel sounds o Nausea, vomiting, constipation, abdominal distention o Paralytic ileus
Nursing Interventions
E CG changes (Tall T wave), E dema R eflexes (hyperreflexia or areflexia)
Nursing Interventions Assess o VS o I & O Monitor o K+ Administer o Diuretic o Dextrose or Glucose Perform o Cardiac monitor Teach o Avoid POTASSIUM
What foods are high in POTASSIUM? P otatoes & Pork O ranges T omatoes A vocadoes S trawberries S pinach f I sh m U shrooms M elons Cantaloupes
If the K+ is too high during an infusion, stop the infusion and call the provider.
*Magnesium Helps with muscle relaxation Normal levels: 1 – 2.
Hypomagnesemia (less than 1) *Muscles are excited
Risk factors/causes of Hypomagnesemia
Remember “LOW MAG” L imited intake of Mg+ (starvation) O ther electrolyte issues cause low Mg+ W asting Mg+ via the GI (Diarrhea, NG suctioning, fistula drainage) M alabsorption issues (anorexia) A lcohol (chronic alcoholism) G lycemic issues Diuretics
Expected clinical manifestations
Remember “TWITCHING” T ovessau’s sign (positive) W eak respirations I rritability T ardive Dyskinesia, Twitching, Tetany C ardiac changes (Tachycardia, EKG changes: Widened QRS, prolonged PR & QT intervals, depressed ST segments, broad flattened T waves, prominent U wave) H ypertension, Hyperreflexia (Increased DTR) I nvoluntary movements N ausea G I issues
Difficulty swallowing, Paralytic ileus, Nystagmus (eye twitching)
Nursing Interventions Assess o VS (tachycardia & tachypnea) Monitor o Magnesium levels Administer o Magnesium Perform o Teach o Foods that are rich in Magnesium
Always Get Plenty Of Foods Containing Large Numbers Of Magnesium A vocado G reen leafy vegetables P eanut butter; pork O atmeal F ish
Sodium (135 – 145) *Sodium is sensitive to fluid
Hyponatremia (less than 135) When Na+ is low then there is an excess in fluid
Risk factor/Causes
Remember “No Na+” N a+ excretion increased with renal problems, NG suction, vomiting, diuretics, sweating, diabetes insipidus O verload of fluids (CHF, Hypotonic fluids, liver failure) N a+ intake low A ntidiuretic hormone over secreted
Clinical manifestations of hyponatremia
Remember “SALT LOSS” S eizures & Stupor A bdominal cramping & attitude changes (confusion) L ethargy T endon reflexes L oss of urine and appetite (nausea, vomiting, anorexia) O rthostatic hypotension S hallow respirations S pasms of muscles Headache
Nursing Interventions Assess o LOC o VS Monitor o Electrolytes (Na+) Administer o Hypertonic solution Perform o Fall risk Teach o Eat foods with salt
Hypernatremia (more than 145) *High Na+ but low water so the patient is dehydrated
Risk factors/Causes
Remember “HIGH SALT” H ypercortisolism (Cushing syndrome), Hyperventilation & Heat stroke I ncreased Na+ intake (oral or IV routes) G I feeding without adequate H20 supplement H ypertonic solutions S odium excretion is decreased A ldosterone problems L oss of fluids (dehydration) T hirst impairment
Clinical manifestations of hypernatremia
Remember no “FRIED” foods for you F ever, flushed skin R estlessness, really agitated I ncreased fluid retention E dema, extremely confused D ecreased urine output, dry mouth/skin Furrow tongue
Nursing Interventions Assess o VS Monitor o Na+ o EKG Administer o Hypotonic o Diuretic Perform o Reposition Q o Weigh daily Teach o Have them eat less salt
Adult Health 1 Quiz 1
Course: Adult Health I (NR-324)
University: Chamberlain University

- Discover more from: