- Information
- AI Chat
Jennifer Hoffman - VSIM
Nursing Care of the Childbearing Family (NURS 125)
Raritan Valley Community College
Recommended for you
Preview text
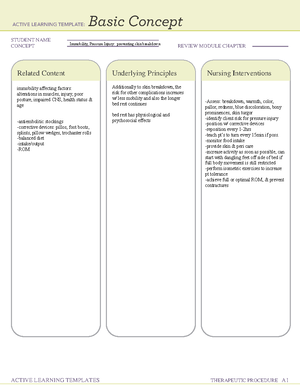
CONCEPT MAP WORKSHEET
####### DESCRIBE DISEASE PROCESS AFFECTING PATIENT
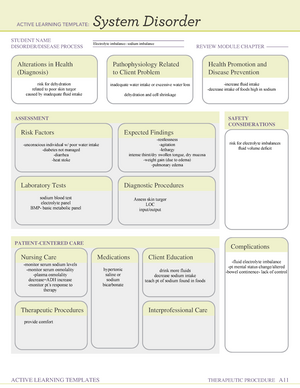
(Include Pathophysiology of Disease Process) Asthma- chronic disease that affects the lungs, causing its airways to narrow as they get inflamed, which makes it hard to breath. It also increases the amount of sticky secretions inside the lung airways. It may also cause trouble talking and being active. Signs and symptoms include: coughing wheezing SOB chest pain & tightness trouble sleeping due to breathing problems all of these symtpoms are a result of airways blockage, inflammation and airway irritability
####### DIAGNOSTIC TESTS
(Reason for Test and Results) ECG to check heart rhythm and abnormalities SpO2 monitoring- bronchoconstriction & bronchial edema may lower SpO2 levels ABGs- asthma can cause respiratory acidosis
####### PATIENT INFORMATION
Jennifer Hoffman Female DOB 1/31/1988 (33y) Height 155 cm Weight 45 kg Allergies: no known Adm on: 2/13/ Adm DX: Acute asthma
####### ANTICIPATED PHYSICAL
####### FINDING
SOB Chest tightness Low pulse oximetry Coughing Wheezing sounds Trouble talking
####### ANTICIPATED NURSING INTERVENTIONS
PT ASSESSMENT VITALS MONITOR SPO2 AND ECG PROVIDE COMFORTABLE POISTION FOR PT BREATHING ADMINISTER MEDICATION OXYGEN ADMINISTRATION AUSCULTATE LUNGS PT EDUCATION OF DISEASE PROCESS & MEDICATIONS
sing
VSIM ISBAR ACTIVITY Student Worksheet
INTRODUCTION
RN Your name, position Emergency Dept. (RN), unit you are working on
SITUATION Jennifer Hoffman, 33YOF
Patient’s name, age, Brought into the ED due to SOB. specific reason for visit
BACKGROUND Adm DX: acute asthma
Orders: Continuous ECG SpO2 monitoring Vital signs every 5min Oxygen to maintain SpO2 above 92% IV normal saline at 150 mL/hour Meds: Albuterol 5 mg in 3 mL normal saline via nebulizer every 20min x 3 doses Iptratropium 500 mcg w/ first dose of albuterol Methylprednisolone 100 mg IV push
Patient’s primary diagnosis, date of admission, current orders for patient
ASSESSMENT Pt appeared to be in respiratory distress. Oriented x3. Tachycardic.
Elevated vitals: SpO2: 71% HR: 103 BP: 124/ Temp: 99 F RR: 31 BPM w/ audible wheezing Skin turgor: normal turgor, skin is bluish, cool to the touch w/ diaphoresis Capillary refill: less than 2 seconds
Current pertinent assessment data using head-to-toe approach, pertinent diagnostics, vital signs.
RECOMMENDATION Follow doctors orders and medications doses as indicated
Any orders or recommendations you may have for this patient
sing
NAME OF MEDICATION, CLASSIFICATION AND INCLUDE PROTOTYPE
MEDICATION: ALBUTEROL
CLASSIFICATION: BRONCHODILATOR
PROTOTYPE: PROVENTIL
SAFE DOSE OR DOSE RANGE, SAFE ROUTE
5 mg in 3 mL normal saline via nebulizer every 20 mins x 3 doses
PURPOSE FOR TAKING THIS MEDICATION
To treat PT’s difficulty breathing, coughing, and chest tightness
PATIENT EDUCATION WHILE TAKING THIS MEDICATION
Immediately report if shortness of breath is not relieved after using medication or if after using medication pt experiences dizziness, palpittions, or chest pain as these are signs of tachycardia which is a known adverse reaction.
PATIENT EDUCATION WORKSHEET
NAME OF MEDICATION, CLASSIFICATION AND INCLUDE PROTOTYPE
sing
MEDICATION: IPRATROPIUM
CLASSIFICATION: BRONCHODILATOR
PROTOTYPE: ATROVENT
SAFE DOSE OR DOSE RANGE, SAFE ROUTE
500 mcg w/ first dose of albuterol
PURPOSE FOR TAKING THIS MEDICATION
Combining albuterol and ipratropium work by relaxing and opening airway passages which makes breathing easier. Combining these medications is used in pt’s with chronic respiratory issues who’s symptoms haven’t been controlled with one medicarion alone
PATIENT EDUCATION WHILE TAKING THIS MEDICATION
How and when to take medication. Immiedately notify dr of chest pain, rash, itching, facial, throat or lower extremity swelling, difficulty breathing and any signs of systemic infection
sing
Nursing Narriative Note:
Include initial head to toe assessment which includes Mentation/LOC, eyes, ears, scalp, skin, neck, heart, lungs, abdomen, pelvic, peripheral, ortho, gait.
Date/time
2/13/
08:43 PM
Pt appeared to be in respiratory distress. Oriented x3. Tachycardic. Elevated vitals: SpO2: 71% HR: 103 BP: 124/ Temp: 99 F RR: 31 BPM w/ audible wheezing Skin turgor: normal turgor, skin is bluish, cool to the touch w/ diaphoresis
sing
####### _
####### NURSING DIAGNOSIS:
Ineffective breathing pattern,
related to swelling and spasm
of the bronchial tubes as
evidence by cough, tachypnea
and using of accessory
muscle.
Activity intolerance
Anxiety
Ineffective airway clarence
Ineffective breathing pattern,
related to swelling and spasm
of the bronchial tubes as
evidence by cough, tachypnea
and using of accessory
muscle.
sing
CLINICAL WORKSHEET
Dat e:
2/13/21 Student Name:
Assigned vSim:
Jennifer hoffman
Initia ls:
Diagnosis: HCP: Isolation: standard
IV Type: peripheral
Critical Labs: Other Services
Ag e:
JH Acute asthma ABG- respiratory M/ acidosis F:
F Length of Stay: Fall Risk: Location: right arm Code Status:
1 day Consults: Consults Needed: Full code Allergies: Transfer: Fluid/Rate: No known 150 mL/hour
Why is your patient in the hospital (Answer in your own words and include the History of present illness)? Pt was brought into the hospital by her neighbor because she was in respiratory distress and was having a hard time breathing and talking Health History/Comorbidities (that relate to this hospitalization): History of asthma for years. Pt has experienced several asthma attacks resulting in hospital visits in the past year
Shift Goals/ Patient Education Needs: 1. Relieve respiratory distress
Improve oxygen saturation
Educate ot on factors that cause flare ups and how to avoid them, such as allergens and environmental factors
Evaluate the patient’s understand of the disease process
Path to Discharge: Upon discharge- SpO2 will remain above 92%, pt will maintain patent airways and will no longer present difficulty breathing, pt will have an understanding of disease process and medication regimen Path to Death or Injury:
sing
CLINICAL WORKSHEET
Alerts:
What are you on Alert for with this patient? (Signs & Symptoms)
Management of Care: What needs to be done for this Patient Today?
Dyspnea, chest tightness, airway blockage
SOB, rapid breathing, confusion, blue lips, skin and fingernails
SOB, chest pain, chills, productive cough, sweating, fatigue, fever
Nebulizer needs to be given to help stabilize oxygen levels
IV medications
Vital signs every 5 mins
Ascultate lung sounds before and after medications are given
Assess to determine treatment effectiveness
Educate pt
What Assessments will you focus on for this patient?
(How will I identify the above signs & symptoms?) 1. Auscultate lungs, as well as physical assessment
Auscultate lungs, as well as physical assessment, assessing pt’s appearance
Pulse ox, sputum test, chest x-ray
List Complications may occur related to dx, procedure, comorbidities:
Priorities for Managing the Patient’s Care Today
Deteriorating of lung function
Respiratory failure
pneumonia
Maintain patent airways
Ascultatue lungs and Monitor vital signs every 5 mins
Obtain health hx
What nursing or medical interventions may prevent the above alert or complications?
What aspects of the patient care can be Delegated and who can do it?
Continuous vital, symptoms & pulse-ox monitoring
Continuous monitoring of respiratory rate
Positioning to promote comfort and better breathing
sing
Last Updated 4/5/
sing
Jennifer Hoffman - VSIM
Course: Nursing Care of the Childbearing Family (NURS 125)
University: Raritan Valley Community College

- Discover more from: